How a Slipped Disc Happens?
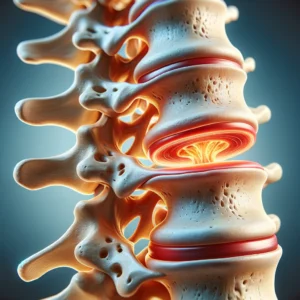
A herniated disk, commonly known as a slipped disc, is a spinal condition that can trigger sharp pain and significantly impact an individual's daily life.
This condition typically arises when the soft, central portion of the spinal disc (the nucleus pulposus) bulges or ruptures through a weakened area in the outer ring, often leading to back pain and discomfort.
When a slipped disc occurs, it can exert pressure on the surrounding nerve roots and spinal cord, contributing to various symptoms.
Who Is At Risk of a Herniated Disk?
Herniated disks occur to anyone, they are not limited to any specific demographic, though certain risk factors, such as maintaining a healthy weight and engaging in proper lifting techniques, can influence their prevalence.
In some cases, a slipped disc can lead to serious conditions like cauda equina syndrome, necessitating immediate spinal surgery.
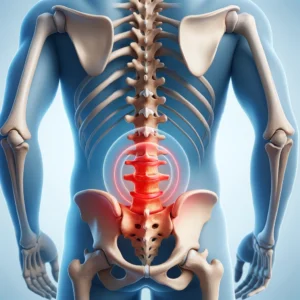
This condition is characterized by a constellation of symptoms including muscle weakness, bladder or bowel incontinence, and severe pain.
For those experiencing a slipped disk, the journey to recovery may involve a variety of treatments. Initial management often includes conservative measures like physical therapy, where a skilled physical therapist guides patients through exercises to improve muscle strength and flexibility. Patients can then continue these exercises at home, which can help manage back pain.
In scenarios where patients feel pain that worsens with movement, an epidural steroid injection may be recommended to alleviate inflammation and discomfort.
Minimally invasive procedures are increasingly becoming a viable option for treating herniated disks, especially when conservative treatments fail.
These include techniques like spinal fusion, where spinal bones are joined to stabilize the affected area, and disk degeneration is addressed.
In cases of cervical radiculopathy, where the slipped disc occurs in the neck region, causing pain that radiates down the arm, a careful physical exam is crucial to determine the exact nerve root affected and the appropriate course of action.
It's important to note that only a small percentage of slipped disc cases require invasive treatments.
Many individuals find relief through other treatments, such as muscle relaxants for spasms, pain medication, and lifestyle modifications like avoiding heavy objects that strain the back muscles.
In rare cases, where conservative management is ineffective, and symptoms persist or worsen, surgery may be recommended.
The key to preventing herniated disks lies in understanding the spine's function as shock absorbers and maintaining its natural curves.
Simple practices like keeping your upper arm and neck forward, standing with your spine curves aligned, and stretching your leg straight can help maintain spinal health.
For those who lift heavy objects regularly, adopting proper lifting techniques—bending at the knees and keeping the object close to your body—can significantly reduce the risk of a slipped disc.
The Mechanics of a Slipped Disc: A Deeper Dive
A slipped disc, often known as a herniated disc, is a common spinal ailment that can cause significant back or neck pain and, in some instances, more severe neurological complications.
Understanding the mechanics of how a slipped disc happens involves a closer look at the spinal cord, spinal canal, and other related structures.
This condition, typically occurring in the lumbar spine, can exert pressure on the spinal nerves, leading to various degrees of discomfort and pain. Remember, you can always contact an expert spine surgeon in Dallas like Dr Baker!
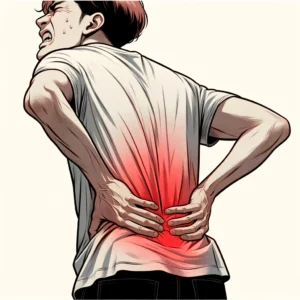
Slipped Disc or Herniated Disc?
A slipped disc, medically referred to as a herniated disc, takes place when the gel-like center of a spinal disc pushes through a crack in the tougher exterior casing. This event can happen in any part of the spine, with the lumbar spine, or lower back, being a frequent site. The herniation can press upon the nerves within the spine, triggering pain and other sensations like numbness or tingling.
Understanding the Spinal Cord and Spinal Canal
The spinal cord plays a critical role as a communication highway, transmitting signals between the brain and the body. It's encased within the spinal column, composed of a series of bones called vertebrae. The spinal canal, a hollow space inside these vertebrae, houses and safeguards the spinal cord. Herniation of a disc can impinge on this canal, potentially affecting the spinal cord or the spinal nerve roots.
Leg Pain and Herniated Discs
When a herniated disc in the lower back impacts the sciatic nerve, it can lead to leg pain, known medically as sciatica. The symptoms can vary from a mild ache to a sharp, burning sensation, and in some cases, muscle weakness in the affected leg. The exact nerve root affected by the herniated lumbar disk determines the nature and severity of the leg pain experienced.
The Lumbar Spine and Herniated Disks
The lumbar spine is comprised of the lower five vertebrae, which support most of the body's weight, making them more prone to disk herniation. Non-surgical treatments, such as physical therapy, are crucial in managing symptoms related to a herniated lumbar disk. A physical therapist can assist in improving muscle strength and flexibility, thus alleviating the discomfort.
When a Slipped Disc Leads to Back or Neck Pain
A herniated disc is often the primary source of back or neck pain, especially when it compresses nearby nerves. This compression can lead to sensations like pain, numbness, or tingling in the body areas served by the affected nerves. The pain experienced can range from a slight downward pressure to more severe, deep pain, impacting daily activities and overall well-being.
Disk Herniation: The Process Explained
The journey towards disk herniation begins with the weakening or degeneration of the disc's outer ring, often due to factors like aging or strain. As the disc weakens, the inner core is more likely to bulge or rupture through the outer ring, leading to herniation.
The Role of Spinal Nerves in Herniated Disks
When herniated disks compress spinal nerves, they can cause pain, numbness, or weakness along the nerve's path. Some individuals experience localized back pain, while others may feel radiating pain down their legs due to specific spinal nerves being involved.
Distinguishing Between Slipped Discs and Other Spinal Conditions
Slipped discs often share symptoms with other spinal conditions, making an accurate diagnosis essential. Healthcare providers use a combination of physical examination, medical history, and imaging tests, such as magnetic resonance imaging (MRI), to differentiate slipped discs from other spinal issues.
Herniated Lumbar Disk and Leg Pain
A herniated disk in the lumbar spine is directly linked to leg pain, particularly if it compresses the sciatic nerve. The pain can manifest as a sharp sensation, muscle weakness, or even deep pain in the leg, depending on the exact nerve root affected.
Back Pain: A Common Symptom of Slipped Discs
Back pain resulting from a slipped disc can be due to direct pressure on the spinal nerves or the body's reaction to the herniated material. Initial treatment often includes rest, pain medication, and physical therapy. In more severe cases, spinal injections or surgery might be recommended.
Navigating the Journey of a Slipped Disc
Treating a slipped disc can often be done with physical therapy, improving your muscle strength and muscle reflexes can help strengthen the stabilizing muscles around your spinal discs. If it progresses then it can be addressed using a minimally invasive procedure should a qualified surgeon recommend surgery.
Understanding how a slipped disc occurs is crucial in addressing and managing this condition. While it can cause significant discomfort and disruption, the right combination of medical intervention, physical therapy, and lifestyle adjustments can lead to effective management and relief from symptoms.
Through this detailed exploration of the mechanics of a slipped disc, we gain a clearer understanding of its impact on the spinal cord, spinal canal, and surrounding nerves.
The intricate interplay between these structures underlines the importance of a comprehensive approach to diagnosis and treatment.
By recognizing the signs and seeking timely medical attention, individuals can navigate the challenges posed by a slipped disc and work towards recovery and pain relief.
Dr. Abdul Baker - An Expert Neurosurgeon in Texas
Every neurosurgery has its complications; thus, a patient must choose the best neurosurgeon for himself. Dr. Abdul Baker is one of the most experienced and qualified neurosurgeons in Texas, treating patients for more than 16 years. People in Sherman, Plano, and nearby areas trust him for every kind of neurosurgery due to his surgical procedures’ 100% success rate. You may visit him if you need any consultancy or treatment regarding your brain and spine disorders.


Dr. Baker specializes in neurosurgery, neurosurgical spine surgery, neurotrauma, brain tumors, spinal tumors, and peripheral nerve damage treatment.